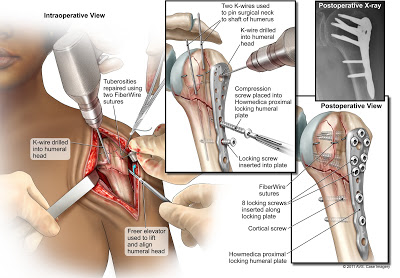
In addition to biological considerations with ORIF, it is critically important that mechanical/surgical failures are avoided. These are factors that we consider prior to undertaking ORIF. Increasing comminution and displacement of the tuberosity segments, head dislocation, and a short calcar segment have been reliably and reproducibly correlated with avascular necrosis. Most biological failures in our series were related to avascular necrosis, which is related to perfusion of the head segment ( 1). Middle-age (40–60 YO) patients with complex medical comorbidities that would lead to a high rate of failure and avascular necrosis (dialysis, transplant, severe diabetes, etc.).Īvoiding ORIF in this patient group will lead to a substantial decrease in biological failures.ORIF, open reduction and internal fixation. 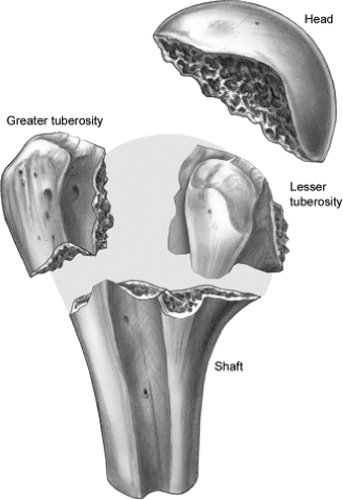
We would favor reverse total shoulder arthroplasty over ORIF for this patient. Elderly patients, with three- and four-part fractures ( Figure 1A,B) įigure 2 Grashey (A) and axillary lateral (B) radiographs of a four-part posterior fracture dislocation in a 56-year-old male.In our practice, we avoid ORIF for patients with the following characteristics: For this reason, the first critical decision is whether a patient is a candidate for ORIF. While mechanical failures were rare, biological failures were common, particularly in three- and four-part fractures in the elderly. At our institution, we recently reviewed the failure rate of ORIF in a series of elderly patients. While avoidance of infection cannot always be obtained, biological and mechanical complications, in our opinion, can be mitigated. It is our opinion that with careful patient selection, a principal based surgical technique, and close postoperative management, complications and re-operations in the setting can be minimized.Īs described, complications can be mechanical, biological, or infectious. While postoperative management of the failed ORIF of a PHF can lead to improved outcomes, it is undoubtedly better to avoid this complication primarily. The goals of this review include a discussion of mechanisms of avoidance of complications after ORIF of PHFs, as well as a description of mechanisms of treatment to salvage this difficult situation. This may be enabled with careful patient selection, a principle-based surgical technique, and close postoperative management. The first priority in management of complications is avoidance. In this setting, the rate can be as high as 30–40% ( 1- 5).įailures of proximal humeral locking plates can be mechanical, biological, or infectious. This was especially true in the setting of elderly fractures, particularly three- and four-part fractures. However, complications associated with use of this technology became rapidly apparent. The advent of proximal humeral locking plates led to increased enthusiasm and utilization in the setting of open reduction and internal fixation (ORIF) of displaced proximal humerus fractures (PHFs). Received: 23 April 2020 Accepted: Published: 15 April 2021. Keywords: Shoulder fracture proximal humerus fracture (PHF) reverse total shoulder arthroplasty (rTSA) open reduction and internal fixation (ORIF) In very rare cases, fusion may be needed. Ensuring appropriate component position, as well as healing of the tuberosities will improve functional outcomes and decrease complications of rTSA. For the majority of patients, revision to reverse total shoulder arthroplasty (rTSA) will be the most reliable treatment option. In select young patients with an intact rotator cuff, hemiarthroplasty may be a viable option. In young patients with preserved bone stock and humeral head anatomy, revision open reduction, internal fixation can be contemplated. Issues with any of these will define management options. Special attention needs to be paid to axillary nerve function, bone loss, rotator cuff function, and infection. Obtaining outside operative reports can help clarify decision making of previous surgeons. This includes patient history, physical exam, plain film radiographs, CT scans, and in some cases further advanced testing (EMG and/or aspiration). In the setting of failure, a thorough workup is needed to evaluate causes of failure and treatment options. Appropriate patient selection, a principle-based surgical technique, and conservative postoperative restrictions can help minimize failures. Failure rates, however, remain high, particularly in elderly patients with complex and severe PHFs. Policy of Dealing with Allegations of Research MisconductĪbstract: The introduction of fixed angle locking plates increased the frequency and reliability of fixation of proximal humerus fractures (PHFs).Policy of Screening for Plagiarism Process.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
